Start exploring drug and alcohol rehabs today. Treatment providers are available to answer your questions.
Painkillers are drugs that are used to treat pain. They are also known as analgesics, pain relievers, or pain medicines. There are various types of painkillers available, each with its own brand name.
The term “pain killer” has been applied to various substances that relieve pain by multiple mechanisms. The most common types include:
Opioids are natural products derived from opium, such as morphine, codeine, and heroin. These compounds affect opioid receptors located throughout the body. Opioid receptor sites are found in the brain, spinal cord, gut, heart, lungs, kidneys, pancreas and reproductive organs.
Non-opioids are synthetic chemicals with similar effects to opioids but with less addictive properties. Examples include aspirin, ibuprofen, paracetamol and tramadol.
Nonsteroidal anti-inflammatory drugs are a class of medications that reduce inflammation and decrease pain. Common examples include aspirin, ibuprofen and naproxen.
Other classes of painkillers include anticonvulsants, antidepressants, muscle relaxants and topical agents.

Oral Route – The oral route is the most common method of administering painkillers. It involves swallowing a pill, capsule or liquid form.
Sublingual Route – A sublingual tablet dissolves quickly on the tongue and rapidly enters the bloodstream. Sublingual tablets are usually used for short term treatment.
Intravenous Route – Intravenous injections are given by inserting a needle into a vein in the arm.
Rectal Route – Rectal suppositories can be inserted into the rectum. These are usually used for long term treatment.
Topical Route – Topical creams, ointments and gels are applied to the skin. They are usually used for treating minor aches and pains.
Intranasal Route – Nasal sprays are sprayed up each nostril. They are usually used to treat sinus infections.
Painkillers can be used to manage pain in many medical conditions. Below are just a few examples:
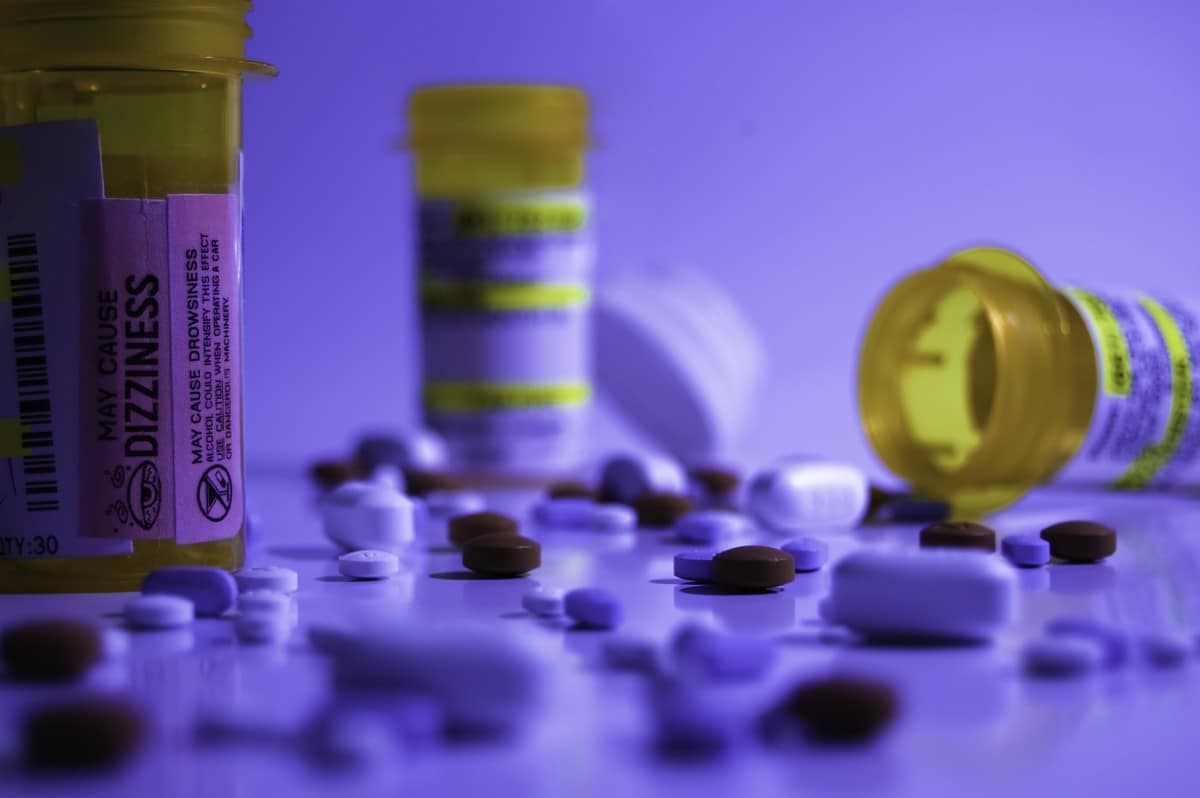
Opioid painkillers are powerful prescription medicines that act in the central nervous system to produce a calming effect. They work by binding to specific areas of the brain called opiate receptors. This causes them to slow down activity in the CNS.
Opioids can be divided into two groups based on their chemical structure:
Endogenous opioids are naturally occurring opioid peptides produced by the human body.
Endogenous opioids include endorphins, enkephalins, dynorphins, nociceptin/orphanin FQ and beta-endorphin.
Synthetic opioids – these are manmade versions of endogenous opioids.
Synthetic opioid painkillers include oxycodone, hydrocodone and fentanyl.
Opioid Painkillers are the most commonly abused type of painkiller.
If you or a loved one has a problem with Painkillers, give us a call on 0800 999 1083, and we can help you find treatment.
Morphine is one of the oldest and best known of all anaesthetics. It is also one of the strongest. Morphine relieves pain by binding to opioid receptors in the brain and spinal cord. This causes changes in the way nerve cells communicate with each other.
Codeine is chemically related to morphine, although it does not bind to opioid receptors.
Hydrocodone – this is another commonly prescribed opioid painkiller. It works just like morphine but is less potent.
Fentanyl – is a powerful narcotic painkiller that acts directly on the central nervous system. Fentanyl can be injected into the bloodstream through a needle placed near a vein.
Oxycodone – this is a semi-synthetic form of morphine. It is available in tablet form for oral use.
Hydromorphone is a highly effective opioid painkiller that is often given when other forms of treatment fail. It comes in tablet form for oral administration.
Methadone – is a long-acting opioid painkiller that is administered orally. It is used to treat people who suffer from severe chronic pain due to cancer or AIDS.
Dilaudid is a short-acting opioid painkiller that comes in pill form for oral ingestion.
Tramadol is a newer type of opioid medication that combines both mild opiate and NSAID painkilling action. Tramadol is usually taken once or twice daily.
Ketamine is a sedative/anaesthetic agent that produces its effects by stimulating opioid receptors. Ketamine is sometimes used to help patients suffering from acute pain.
Ketobemidone – this is a combination product containing ketamine and buprenorphine. Ketamine is a dissociative anaesthetic that reduces anxiety and depression. Buprenorphine is a partial agonist at mu-opioid receptors and is used to treat moderate to severe pain.
Buprenorphine – this is a partial agonist opioid that is used to treat moderate and severe pain.
Butorphanol – is a strong opioid painkiller used to relieve moderate to severe pain. Butorphanol is a derivative of thebaine, which is extracted from the coca plant.
Nalbuphine – is a weak opioid painkiller that is similar to morphine. Nalbuphine is used to control moderate to severe pain.
Tapentadol – this is an extended-release formulation of oxycodone. Tapentadol is approved as an adjunct therapy for managing moderate to severe pain. The recommended dose is 50 mg every 4 hours.
Percocet is a combination of acetaminophen and oxycodone, a prescription painkiller. Percocet contains 325mg of acetaminophen and 5mg of oxycodone.
Vicodin – is a combination drug containing hydrocodone and acetaminophen. Vicodin has been shown to reduce pain more effectively than either component alone.
If you or a loved one has a problem with Painkillers, give us a call on 0800 999 1083, and we can help you find treatment.
Speak to us on 0800 999 1083 to discuss treatment options and to find the best alcohol rehab centre.
All painkillers work in one way or another to block the transmission of pain signals between the nerves and the brain. This means they can be effective against both acute and chronic pain.
Acute pain occurs when you injure yourself, for example, if you cut your finger.
Chronic pain occurs over time, for example, arthritis. Chronic pain is often caused by nerve damage, which leads to changes in the nervous system.
There are two main ways painkillers work:
They either act directly on the nerve endings themselves, or they alter the activity of the central nervous system, which controls all other parts of the body.
Indirect Acting Analgesics
This includes aspirin, ibuprofen and paracetamol. They work by reducing the number of inflammatory substances produced by cells in the body. This reduces the level of pain felt by the person.
Direct Acting Analgesics
These include morphine, codeine, oxycodone, hydrocodone and fentanyl. They all work by binding to receptors in the brain that control pain.
Neurolytics work by blocking the release of neurotransmitters at the site of injury or irritation.
Narcotics work by binding to specific receptors in the brain and spinal cord.
Opioids bind to three different opioid receptors: mu, delta and kappa. Mu receptors are located mainly in the brain and spinal column; delta receptors are present in the brain stem and spinal cord; and kappa receptors are found in the brain stem, spinal cord and peripheral tissues.
These receptors are activated by opioid peptides produced naturally within the body. When released into the bloodstream, these peptides cause several physiological responses, including dilation of blood vessels, constriction of airways, and central nervous system stimulation.
When taken orally, opioid drugs must first pass through the liver before reaching their target in the brain. This process causes them to lose much of their potency.
Opioids work by interacting with specific proteins called opioid receptors located throughout the body.
The most important function of these receptors is to regulate bodily functions, including breathing, digestion, blood pressure, reproduction, sleep, temperature regulation, immune response, and mood. In addition to regulating normal physiological processes, opioids also can produce feelings of pleasure. Therefore, they play a role in our emotional well being.
When we experience pain, our bodies release chemicals that activate opioid receptors.
When activated, these receptors send signals to the brain’s reward centres. This causes us to feel pleasure.
However, if you take too many of these opioid medications, your body will eventually develop tolerance to them. Tolerance means that your body requires higher drug doses to get the same effect. Once your body becomes tolerant to one particular opioid, it can become resistant to all opioids.
This is why many people who use opioid painkillers find themselves addicted to them.
Opioid addiction occurs when repeated use of a substance leads to physical dependence and withdrawal symptoms if the substance is stopped suddenly. Physical dependence refers to the need for continued use of the substance to get the same effect.
When you take pain killers like Oxycontin, Vicodin, or Percocet., it’s not uncommon for your body to become dependent on these drugs. When you stop taking them, withdrawal symptoms will occur. This prescription drug addiction‘s most common side effects include nausea, vomiting, diarrhoea, muscle aches, anxiety, insomnia, and depression. If you experience any of these symptoms while trying to quit cold turkey, it could be because you have formed a physical dependence on the drug.
Talk with your doctor (or an addiction specialist) about whether or not you should take prescribed painkillers. Your doctor can tell if you have a legitimate need for painkillers based on how severe your injuries are. They may recommend alternative therapies instead.
The most important thing to remember about taking painkillers is that you should only take them when you really need them. If you don’t feel like you need it, then don’t take it!
If you do decide to take a painkiller, make sure you follow the instructions provided by your doctor carefully. You may not be able to use specific combinations of medicines safely.
It’s also important to avoid mixing prescription medication with alcohol or illicit drugs. Doing so could result in serious health problems.
In addition, if you have been prescribed more than one type of painkiller, always check with your doctor before switching to a new medicine.
Always follow the directions on the label. Do not take more than the prescribed dose.
Some medications can help reduce cravings for painkillers. Talk to your doctor about these medications. If you have a prescription painkiller addiction, talk with your doctor about getting off them.
If you or a loved one has a problem with Painkillers, give us a call on 0800 999 1083, and we can help you find treatment.
The term “addict” is often used to describe someone who takes painkillers repeatedly and habitually. However, addiction is a complex issue, and there are no simple answers. There are two main types of addiction: physical and psychological.
Abuse of painkillers can lead to dependence and addiction.
Dependence occurs when your body becomes accustomed to the effects of pain killers.
When this happens, you need more and more of the medication to produce the same level of pain reduction.
Withdrawal Symptoms
Unpleasant withdrawal symptoms occur when you stop taking painkillers. These can range from mild discomfort to severe complications like seizures. Your doctor will advise you on the best way to withdraw safely.
Toxicity
Overdose is another risk associated with painkillers abuse. Overdoses can result in coma and death.
People who overdose are likely to suffer from nausea, vomiting, dizziness, confusion and hallucinations.
Toxic levels of painkillers can build up in your system. When this happens, you’re at greater risk of developing an addiction.
If you suspect yourself or a loved one is overdosing on painkillers, please call 999 immediately!
Physical dependence is when your body gets used to the effect of a drug.
This means that even though you’ve stopped taking the drug, your body still reacts as if it were still there. Physical dependence usually develops within two weeks of starting to take painkillers.
After that time, you should be able to reduce or stop taking the medication.
Physical dependence does not mean that you’re addicted to painkillers. However, it may make withdrawal more difficult.
Psychological dependence refers to a psychological state where you feel compelled to use painkillers.
You may have developed a habit of taking painkillers for reasons such as stress, anxiety or depression.
In these cases, you may find yourself unable to function without painkillers.
Psychological dependence is different from physical dependence. You may continue to experience withdrawal symptoms even after stopping the medication.
Tolerance is a physiological response to repeated exposure to a substance.
As tolerance builds, the number of painkillers needed to get the desired effect increases.
If you take too many painkillers over a short period of time, you may develop tolerance. This makes it harder to control how many painkillers you take.
Withdrawal syndrome is a set of unpleasant symptoms experienced by someone withdrawing from chronic use of painkillers. These include:
If you suspect yourself or a loved one is experiencing serious effects of painkillers withdrawal, please call 999 immediately!
There are many different Risk factors of painkillers addiction. Some of the most common include:
Prescription Misuse: Prescription misuse occurs when someone takes prescription painkillers for nonmedical reasons. For example, a person could take painkillers after surgery because they believe that they will help ease postoperative discomfort. Or, a patient could take painkillers for recreational purposes such as to enhance sexual pleasure.
Overprescribing: Overprescribing refers to prescribing too many painkillers for a particular condition. One study found that approximately 50% of those suffering from chronic back pain were given unnecessary medication.
Taking large amounts of painkillers at once: Taking too many painkillers at one time increases the likelihood of becoming dependent on the substance.
Using painkillers recreationally: Recreational use of painkillers is another factor that increases the chance of developing an addiction.
Although genetic factors play a role in painkiller abuse and addiction, environmental factors are just as important. Some people are genetically predisposed to develop addictions, while others are not. This means that certain individuals are more likely to become addicted to painkillers than others.
Genes play a significant role in determining whether you are susceptible to addiction. Two types of genes influence your susceptibility to addiction:
Dopamine Receptor D2 Gene: People who inherit this gene are more likely to suffer from addiction because they tend to experience intense cravings when exposed to dopamine-producing drugs such as cocaine, heroin, and alcohol.
Serotonin Transporter 1A Gene: People who inherit this gene tend to show signs of withdrawal after they stop taking painkillers.
Environmental factors include things like social support systems, family history, peer pressure, and access to painkillers. These factors can either make you more prone to addiction or protect you against it.
Social Support System: If you live in a household with little tolerance for substance abuse, you will probably be less likely to develop an addiction.
Family History: If you have a family history of substance abuse, you are more likely to become dependent on painkillers.
Peer Pressure: Peer pressure can be very influential in shaping your decision to take painkillers. For example, if you see someone else abusing painkillers, you might decide to try them too.
Access to Painkillers: If you live in an area where painkillers are readily available, you are more apt to use them.
People who are prescribed painkillers by their doctor are most at risk of developing a painkillers addiction. However, anyone who uses painkillers recreationally is also vulnerable to addiction.
Those who are prescribed painkillers should only take them under the supervision of a doctor. Do not share your medication with friends or relatives under any circumstances.
If you struggle with painkiller addiction, seek help today. We can help you find the right treatment programs for you that provide comprehensive care and individualised treatment plans designed to meet your specific needs. Call us now at 0800 999 1083 to learn more about how we can help you overcome your painkiller addiction.
The signs of a painkillers addiction may vary depending on whether you are addicted to opiates or non-opiate painkillers.
With opioid dependence, you will experience physical cravings for the drug. These cravings can cause you to do things like lie to your doctor about missing doses of the medication.
Opioid withdrawal symptoms usually occur within 24 hours after stopping taking the medication. Common withdrawal symptoms include sweating, shaking, vomiting, diarrhoea, stomach cramps, restlessness, headache, depression, irritability, sleep problems, mood swings, difficulty concentrating, and increased appetite.
Non-opioid dependency is characterised by an intense desire to use painkillers again. People suffering from this type of addiction often have trouble controlling their behaviour. They may be unable to function normally without the medication.
In addition to experiencing physical cravings, those who suffer from withdrawal symptoms associated with non-opioids develop psychological cravings as well. For example, they might become preoccupied with thoughts of the drug. They may also experience feelings of guilt and shame.
Physical signs of painkillers addiction include:
Psychological signs of painkillers addiction can be difficult to detect. However, there are specific indicators that you should watch out for. These include:
Behavioural symptoms of painkillers addiction include the following:
If you stop taking painkillers suddenly, you may experience withdrawal symptoms such as:
If you or a loved one has a problem with Painkillers, give us a call on 0800 999 1083, and we can help you find treatment.
The dangers associated with painkillers addiction and abuse include:
Addiction to painkillers is a serious problem that needs immediate attention. If you suspect that you have an addiction, seek help immediately. Call us on 0800 999 1083 to discuss treatment options.
All painkillers carry risks. Some of these are listed below.
Some people become addicted to painkillers. This means their tolerance to the drug increases over time.
Overdosing on painkillers can cause serious health problems. If someone has overdosed on painkillers, it is crucial to call 999 immediately!
Respiratory depression occurs when the respiratory system stops working properly. This may lead to death, so please call 999 immediately!
Kidneys damage can occur as a result of taking too many painkillers.
Heart problems can also arise due to taking too many painkillers, particularly if they contain alcohol.
Taking large amounts of painkillers can increase the risk of seizures. It is best to avoid this by not mixing different types of painkillers.
People who take high doses of painkillers can experience memory loss.
Drug interactions can occur when you combine painkillers. These can make your condition worse.
For example, combining paracetamol with caffeine can cause liver toxicity. It is best to stick to one type of painkiller at a time. If you are prescribed more than one painkiller, always read the instructions carefully.
Some people who abuse painkillers also abuse other types of drugs. For example, they might combine painkillers with alcohol or sedatives. Some people who abuse painkillers may also use them to self-medicate depression or anxiety. It is essential to know if you are abusing painkillers along with another substance. It is best to talk to your doctor about what you are doing.
In general, people who abuse painkillers may also abuse alcohol or illegal substances. If you’re worried about abusing painkillers, talk to your doctor. They can recommend ways to manage your pain without relying on addictive drugs.
Overdose symptoms vary depending on the type of painkiller taken. For example, if you overdose on Vicodin, you might get drowsiness, nausea, vomiting, constipation, confusion, dizziness, hallucinations, seizures, or coma.
If you overdose on OxyContin, you could get nausea, vomiting, stomach cramps, sweating, weakness, slurred speech, breathing difficulties, or unconsciousness.
Other common signs of an opioid overdose include dilated pupils, pinpoint pupils, dry mouth, cold/clammy skin, shallow breathing, slow pulse, and shallow breathing.
If you think you might have taken too much, call 999 immediately. Do not drive yourself to the emergency room if you suspect an overdose.
There are many things you can do to prevent an opioid overdose. Here are a few tips:
Never mix alcohol with opioids. Mixing alcohol with opioids can make it harder to tell whether you’re overdosing.
Don’t take too large a dose at once. Taking a small dose every hour instead of a big dose all at once can help keep you safe.
Keep track of your doses. Keep a log of how many pills you’ve taken and when. Write down the date, time, and reason why you took each pill.
Call 999 immediately if you think someone else may be overdosing on painkillers.
Opioid abuse can cause depression, anxiety, agitation, restlessness, insomnia, and suicidal thoughts. These side effects can increase your risk of suicide. Talk to your doctor right away if you experience these symptoms.
If you are thinking about harming yourself, please call 0800 999 1083 now.! Your life matters. You deserve to live it free from pain.
Addiction to painkillers can impact relationships in many different ways. When someone becomes addicted to painkillers, it can change how they interact with others:

Co-occurring disorders refer to mental illnesses that occur along with another diagnosis, such as drug use disorder. Mental health disorders often co-occur with addiction. Some people who struggle with addiction also suffer from depression, bipolar disorder, posttraumatic stress disorder, anxiety, eating disorders, attention deficit hyperactivity disorder, obsessive-compulsive disorder, personality disorders, schizophrenia, and others.
When two conditions co-exist, they can interact with one another and lead to more severe problems. For example, depression can worsen addiction by making it difficult for people to stop using drugs. Similarly, addiction can trigger intense mood swings that can last for days.
Some people who struggle with addiction develop physical changes in their brains due to long-term drug use. This leads to brain damage, which can cause cognitive impairment and other problems. People who develop prescription mental illness before prescribing pain killers.
Dual diagnoses are common among people struggling with addiction. A dual diagnosis refers to having both a mental health condition and a substance use disorder. Most people with a dual diagnosis have experienced trauma in their lives. Trauma can lead to emotional distress, which can then become a trigger for addictive behaviour.
Many people with a dual diagnosis seek treatment for both substance abuse and mental health issues. Treatment programs for dual diagnoses usually combine medication and therapy.
Coping strategies are ways we deal with stressful situations. Many people turn to painkillers to cope with painful emotions. When this happens, they end up suffering from an addiction.
While coping strategies are helpful at times, they can also become unhealthy habits. If you find yourself turning to painkillers because you feel overwhelmed by negative feelings, talk to your family members, friends, or doctor about what’s going on.
You don’t have to keep living like this. There’s help available. Call us on 0800 999 1083 to discuss treatment options.
If your loved one needs support dealing with an Alcohol Addiction, contact us today on 0800 999 1083. We can help you by recommending treatment options.
In teens, painkillers addiction may be triggered by traumatic events, such as sexual assault, bullying, or car accidents. It may also stem from chronic medical conditions like arthritis, migraines, or fibromyalgia.
The most common type of teen painkiller addiction involves abusing opioid pain relievers, such as OxyContin and Vicodin. These pills contain opioids, which are potent chemicals that relieve pain.
If you’re addicted to painkillers, you might start taking larger amounts than prescribed. You could even take more than your doctor prescribes. This behaviour can lead to overdose. Overdoses can cause hallucinations, seizures, coma, or death. Call 999 immediately if you think you or someone else may be overdosing on painkillers. You should also talk to your family and friends about your painkillers abuse.
Talk to your child’s doctor. You may want to ask questions like:
People who want to help their loved ones with painkillers addiction need to understand why they started using the drug.
They should also know if there are signs that the person has developed a dependence on painkillers.
If the person is willing to accept help, the following steps can help:
Talk to the person about their use of painkillers. Ask questions so that you can better understand the situation.
Encourage the person to seek professional help.
Help the person deal with underlying emotional problems.
You may notice signs of painkillers misuse in others. Look for the following:
If your loved one doesn’t admit they have a problem or refuses to get treatment for the painkillers addiction, then you may have to stage an intervention.
This is a formal meeting where everyone agrees to support the person’s decision to quit painkillers.
Here are some tips for staging an effective intervention:
Make sure all those present agree to support the person’s recovery.
Let the person know that you love them no matter how difficult the decision might be.
Show respect by listening carefully to the person’s reasons for continuing to use painkillers.
Give the person as much time as needed to decide whether to continue using painkillers.
Do not argue with the person.
Contact a doctor or therapist to help the person through the withdrawal process if necessary.

There are many different treatments available for people who suffer from painkillers addiction. You don’t have to keep living like this. There’s help available. Call us on 0800 999 1083 to discuss treatment options.
Seek emergency medical help when a loved one shows symptoms of overdose. Call 99 immediately!
Speak to us on 0800 999 1083 to discuss treatment options and to find the best alcohol rehab centre.
Once a person decides to get treatment for painkillers addiction, several options are available. Call us on 0800 999 1083 to discuss treatment options.
People addicted to painkillers often exhibit certain behaviours that indicate their problems.
The most common signs of painkillers addiction are:
Once you’re diagnosed with a Painkiller Addiction, an individual rehab program can be created to help you recover.
Withdrawal symptoms occur after someone stops taking painkillers.
Detoxification refers to the process of getting rid of the physical toxins leftover from abusing painkillers.
After detoxification, it is possible to begin an individualised recovery plan. This will involve finding a suitable program that meets your needs. Some people choose to go to rehab centres. Others prefer outpatient programs. You may need to stay at an inpatient facility for a few weeks or months.
Your treatment team can help you find the right place for you.

Inpatient rehabilitation programs are usually located in hospitals or clinics.
They provide intensive therapy and treatment for people suffering from drug abuse problems.
The goal of these programs is to teach patients about their problems and help them learn ways to cope with them.
People who participate in inpatient rehabilitation programs often find they need to stay longer than they expected.
Outpatient rehabilitation programs are offered at local health facilities.
They offer less intense therapy than inpatient programs, but they still require participants to attend regularly scheduled sessions.
Medication-assisted treatment (MAT) successfully treats both the physical and psychological components of painkiller addiction when used in conjunction with psychotherapy.
Methadone, for example, can help with cravings and withdrawal symptoms.
Buprenorphine works by partially activating opioid receptors in the brain, preventing overdose and the pleasure associated with substance dependence.
Don’t go through the process of recovery alone. Treatment providers can answer your questions. Get in touch with one today.
Call 0800 999 1083 today!
The most important part of treatment is therapy. It’s also called counselling, psychotherapy, or talk therapy. You’ll likely meet with a therapist several times a week when you’re going through rehab. They will provide you with support and guidance throughout your recovery process.

There are several ways in which therapy can help you:
The goal of both individual and group therapy is to improve treatment outcomes. Individualised therapy is a one-on-one talk therapy in which you meet with your therapist alone. You’ll learn to understand your addiction, recognise triggers, and develop coping strategies during these sessions.
While in recovery, group therapy is an excellent place to meet new sober friends and receive support and feedback. A qualified drug counsellor leads group therapy sessions, including several recovering addicts. The knowledge you gain during the sessions will assist you in avoiding triggers and preventing relapse.
Addiction to painkillers is a serious problem that needs immediate attention. Call us on 0800 999 1083 to discuss treatment options.

Once you complete your treatment plan, you’ll likely begin working toward long term sobriety.
To prevent relapse, you need to be committed to staying sober. This means avoiding situations where you might be tempted to use again. These include places where you might find yourself alone, like your car or house.
Call someone right away if you feel like you’re about to drink or take painkillers. Don’t wait until you’re ready to use. Also, don’t keep secrets from those close to you. Tell everyone you trust about your struggles with addiction and ask them to be supportive. Let them know if you think you’re having trouble controlling your urge to take painkillers.
If you’re concerned about your ability to stay sober, ask your doctor for advice:
They can recommend resources that can help you cope with cravings and urges.
A counsellor can help you work through your feelings and concerns while participating in meetings. They can also give you tips on preparing for stressful life events. For example, they may suggest learning relaxation techniques, like meditation. Or maybe your doctor will recommend joining a 12-step program. In this case, it would be helpful to speak with a counsellor simultaneously.
Narcotics Anonymous and SMART Recovery are two community-based support groups where you may talk about your addiction and learn practical coping methods from the shared experiences of other recovering addicts. The main distinction is that NA attributes healing to a higher power, whereas SMART Recovery does not.
Don’t go through the process of recovery alone. Treatment providers can answer your questions. Get in touch with one today.
Call 0800 999 1083 today!
According to the National Statistics, the following data refer to the period 2019-2020.
The number of persons seeking treatment for opiate addiction remained stable from the previous year (going up slightly from 139,845 to 140,599).
In the non-opiate group, there was a 4% increase and a 6% increase in the non-opiate and alcohol group. This follows a slight increase the previous year (2018-2019).
This year, there was a 6% rise in the number of fatalities among opiate addicts in treatment (from 1,897 to 2,010).

BACP accredited psychotherapist with 16 years experience working in mental health specialising in psychodynamic person-centred therapies treating those with a range of mental health disorders including anxiety, depression, OCD and Addiction.

Fill in your details and we’ll send you a message via SMS.


No matter where you live, there are drug and alcohol rehab options for you to discover. Treatment providers are waiting to answer your questions. Get started today.

In our journey towards health and well-being, we often encounter a crossroads between medical treatment and lifestyle choices. The intersection of antibiotics and alcohol is one such area that demands our attention and understanding. Antibiotics, powerful agents against bacterial infections, operate within our bodies to eradicate harmful pathogens. However, when alcohol enters the … Continued

The term addictive personality is often used to describe someone who seems prone to repeated patterns of addictive behaviour. Although it’s not an official psychiatric diagnosis, understanding this concept is crucial in comprehending addiction. It refers to a set of characteristics that may increase the risk of developing addictive behaviours for an individual. In … Continued

By Ana
Embarking on the path to recovery from addiction often involves seeking support from rehabilitation centres, commonly known as “rehab.” This article aims to provide an in-depth exploration of rehabilitation, elucidating the types of rehab centres available in the UK, and delineating the specific programmes tailored for drug addiction and alcoholism, supported by pertinent facts, statistics, … Continued

By Ana
Rehabilitation serves as a beacon of hope for individuals navigating the complexities of recovery. In its essence, rehabilitation represents a transformative journey, encompassing physical, psychological, and social aspects to restore individuals’ well-being. Its significance reverberates across diverse fields, from healthcare to social reintegration, reshaping lives and fostering resilience. Exploring the Meaning of Rehabilitation … Continued

Don’t go through the process of recovery alone. Treatment providers can answer your questions. Get in touch with one today.
Call 0800 999 1083 today!






